From about 8% to 27% of extremely preterm infants
develop symptoms of autism spectrum disorder, but the causes are not
well understood. Preterm infants receive the same doses of the
recommended vaccines and on the same schedule as term infants. The
possible role of vaccination in neurodevelopmental disorders (NDD) among
premature infants is unknown, in part because pre-licensure clinical
trials of pediatric vaccines have excluded ex-preterm infants. This
paper explores the association between preterm birth, vaccination and
NDD, based on a secondary analysis of data from an anonymous survey of
mothers, comparing the birth history and health outcomes of vaccinated
and unvaccinated homeschool children 6 to 12 years of age. A convenience
sample of 666 children was obtained, of which 261 (39%) were
unvaccinated, 7.5% had an NDD (defined as a learning disability,
Attention Deficit Hyperactivity Disorder and/or Autism Spectrum
Disorder), and 7.7% were born preterm. No association was found between
preterm birth and NDD in the absence of vaccination, but vaccination was
significantly associated with NDD in children born at term (OR 2.7, 95%
CI: 1.2, 6.0). However, vaccination coupled with preterm birth was
associated with increasing odds of NDD, ranging from 5.4 (95% CI: 2.5,
11.9) compared to vaccinated but non-preterm children, to 14.5 (95% CI:
5.4, 38.7) compared to children who were neither preterm nor vaccinated.
The results of this pilot study suggest clues to the epidemiology and
causation of NDD but question the safety of current vaccination
practices for preterm infants. Further research is needed to validate
and investigate these associations in order to optimize the impact of
vaccines on children’s health.
prematurity, vaccination, neurodevelopmental disorders, infections, epidemiology, evaluation
Preterm birth (defined as birth occurring before 37
completed weeks of gestation) is known as a major risk factor for
neurodevelopmental deficits, including cerebral palsy, intellectual
disability, cognitive and speech delays, motor deficits, and visual
impairment associated with retinopathy of prematurity. In particular,
preterm birth is the leading cause of neurodevelopmental disorders (NDD)
and disability, including the development of autism spectrum disorder
(ASD) [1-3], but the underlying mechanisms are not well understood.
Preterm infants receive the same doses of the recommended vaccines on
the same schedule as term infants in order to protect them from several
infections [4-7]. However, the possible role of vaccination in the
development of NDD in premature infants has not been assessed, partly
because pre-licensure clinical trials of pediatric vaccines have
routinely excluded ex-preterm infants, and because of the assumed
overall safety of vaccinations [8-15].
This paper presents additional results of a survey
designed to compare the health outcomes of vaccinated and unvaccinated
children educated at home, based on mothers’ anonymous reports on the
birth histories and physician-diagnosed illnesses in their children. The
analysis explores the possible role of vaccination in NDD among
children born preterm.
In 2012, 450,000 babies (11%) were born preterm in
the United States, resulting in 35% of all infant deaths in that year,
more than any other single cause. Worldwide, an estimated 15 million
infants were born preterm in 2010, of which about 13 million survived
beyond the first month. In addition to the acute complications of
prematurity, which include respiratory distress, intracranial
hemorrhage, necrotizing enterocolitis and retinopathy, 345,000 (2.7%)
preterm infants were estimated to have moderate to severe
neurodevelopmental impairment; a further 567,000 (4.4%) had mild
neurodevelopmental impairment, and many more had specific learning or
behavioral disorders [4]. Advances in medical care have led to increased
rates of preterm birth and decreased preterm mortality rates. However,
neurodevelopmental disabilities have increased, especially in infants
born at ≤25 weeks’ gestation, with nearly half of surviving extremely
preterm infants having significant disabilities [16]. Total annual costs
of preterm birth in the United States exceed $26 billion per year, with
an overall average cost of approximately $51,600 per preterm infant
[17].
In a follow-up study of 11-year-old children born
extremely preterm, the rate of ASD was 8% compared to zero percent among
their classmates born at term [18] – a rate at least 5 times higher
than recent population estimates for ASD (14.7 per 1,000, or 1 in 68
children aged 8 years) [19]. In another study involving 84 children born
at <27 weeks of gestation who were screened for ASD at 6.5 years, 23
(27.4%) tested positive for ASD. The ASD-positive group had a
significantly higher frequency of neonatal complications than the
ASD-negative group [20].
Since special efforts are made to vaccinate preterm
infants, the effects of prematurity are difficult to separate from
those of vaccination. Given the benefits of vaccination, it has not been
thought necessary to do so. On the other hand, vaccine safety
assessment in preterm infants is particularly important due to the
frequency of adverse events associated with prematurity itself [21].
Adverse cardiorespiratory events including apnea, bradycardia and
desaturations (oxygen saturation <90%) are well documented following
vaccination in many preterm infants, yet vaccination is strongly
recommended regardless of such events, since the prevention of infection
is considered paramount. Pertussis-containing pediatric vaccines in
particular can increase apnea and bradycardia in ex-preterm infants,
typically after the 2-month dose [22,23]. In a study evaluating the
safety of hexavalent vaccines (DTaP‐IPV‐Hib) involving 78 preterm
infants, vaccination triggered transient cardiorespiratory events in 47%
(15% apnea, 21% bradycardia, 42% desaturations), and those with
pre‐existing cardiorespiratory symptoms had a five- to eight-fold
increased risk of cardiorespiratory events post-vaccination [24].
Age at vaccination of preterm infants is inversely
associated with adverse effects. In one study of 27 preterm infants
vaccinated at ≤70 days of age, 9 (33.3%) developed apnea, bradycardia or
desaturations compared to none among those vaccinated at >70 days of
age [25]. A study of nearly 14,000 extremely low-birth-weight (ELBW)
infants reported a 3.7-fold increase in Rule-Out Sepsis evaluations in
the immediate post-vaccination period as well as high rates of apnea,
bradycardia and intubations [26]. Pre-licensure clinical trials of
pediatric combination vaccines have, however, often specifically
excluded ex-preterm infants, even though these vaccines are routinely
administered to all infants regardless of gestational age at 2, 4 and 6
months of age [27].
At present, over 95% of all U.S. children receive
the CDC-recommended vaccines [28,29] in accordance with the policy that
universal vaccination is essential for maintaining herd immunity [30].
Vaccination is estimated to have prevented millions of illnesses and
hospitalizations and 732,000 premature deaths among U.S. children born
during 1995-2013, at an overall cost savings of $1.38 trillion [31].
Much less is known about the extent and cost of vaccine-associated
injury, which can include severe morbidity and death [32]. Since 1988
over 16,038 claims have been filed with the Vaccine Injury Compensation
Program, which was created in 1986 to compensate individuals and their
families for injuries caused by vaccines. Total compensation paid since
the program began is approximately $3.2 billion [33]. Since only about
one percent of serious vaccine injuries are officially reported [34],
the true extent and cost of vaccine-associated damage on a population
basis is likely to be much higher.
A complicating factor in evaluating the vaccination
program is that individual vaccines against infectious diseases have
nonspecific effects on morbidity and mortality that extend beyond
prevention of the targeted disease. In some instances these effects are
beneficial; in others they increase morbidity and mortality [35]. For
instance, the measles and Bacille Calmette- Guérin (BCG) vaccines
reportedly reduce overall morbidity and mortality [36], whereas the
diphtheria-tetanus-pertussis [37] and the hepatitis B vaccines [38] are
associated with increased morbidity and mortality risks. These
nonspecific effects are consistently reported in studies carried out in
low-income countries but require replication in higher-income
populations.
While the safety of vaccines is officially assured,
observational studies have involved only a limited number of vaccines
and vaccine ingredients, and none has reported on the long-term outcomes
of the present vaccination schedule [39], which has been expanded and
accelerated in recent decades [40]. The current childhood vaccination
program now includes 48 doses of vaccines for 14 diseases from birth to
age 6 years compared to 3 vaccinations for 7 diseases in the 1970s [41].
Given the many unknowns related to the long-term effects of vaccines
and their ingredients, the U.S. Institute of Medicine has recommended
that studies be carried out to compare health outcomes in vaccinated and
unvaccinated groups of children and to determine the cumulative effects
of vaccines [12].
A difficulty in comparing vaccinated and
unvaccinated children has been the apparent absence of a readily
available pool of unvaccinated children. The growing population of
homeschool children (i.e., children educated at home) is a
suitable source for such studies, as vaccination rates are lower in
homeschool children [42]. Homeschool families and children are
approximately representative of US families and children in general,
with an approximately equal median income to that of married-couple
families nationwide, somewhat more years of formal education than
parents in the general population, and a higher average family size of
just over three children compared to the national average of just over
two children [43-45]. Geographically, homeschooling families are
slightly overrepresented in the south; children from all racial/ethnic
backgrounds are involved in homeschooling; about 23% are nonwhite; and
the age distribution of homeschool children in grades K-12 (ages 6 to
18) is similar to that of children nationwide [46]. About 3.4% (1.8
million) of the school-age population was homeschooled in the 2011-2012
school year [47].
An opportunity to address the question of the
possible role of vaccination in NDD associated with preterm birth arose
from the availability of data from a cross-sectional pilot study of the
birth histories and health outcomes of vaccinated and unvaccinated
homeschool children ages 6 to 12, carried out by the authors [48]. The
first aim of the study was to compare vaccinated and unvaccinated
children on a broad range of health outcomes, based on mothers’ reports
in an anonymous online survey. The collected data included
physician-diagnosed acute and chronic illnesses, medications and the use
of health services, as well as pregnancy experiences and birth
histories. The second aim of the study was to determine whether an
association found between vaccination and NDD, if any, remained
significant after controlling for other measured factors.
This report presents additional findings on the
independent association and/or interaction between preterm birth,
vaccination and NDD.
Study planning
A partnership was formed with the National Home
Education Research Institute (NHERI) to carry out the proposed study.
NHERI has been involved in educational research on homeschooling for
many years and has strong and extensive contacts with homeschool
organizations and families throughout the country (www.nheri.org). The study was approved by the Institutional Review Board of Jackson State University.
Study design
The study was cross-sectional in design, aimed at
determining the association between vaccination and health outcomes, and
was based on a survey of homeschooling mothers on the overall health of
their vaccinated and unvaccinated biological children. Contact
information on homeschool families was unavailable. Hence, there was no
defined population or sampling frame from which a randomized study could
be carried out and response rates could be determined. However, the
goal of the pilot study was rather to obtain a convenience sample of
unvaccinated children of sufficient size to test for significant
differences in outcomes between the groups.
We proceeded by selecting 4 states (Florida,
Louisiana, Mississippi, and Oregon) for the survey (Stage 1). NHERI
compiled a list of statewide and local homeschool organizations,
totaling 84 in Florida, 18 in Louisiana, 12 in Mississippi and 17 in
Oregon. Initial contacts were made in June 2012. NHERI sent emails to
the leaders of each statewide organization requesting their support for
the study; this was followed by a second email, explaining the study
purpose and background, which the leaders were asked to forward to their
members (Stage 2). Prospective respondents were provided with a link to
the questionnaire. With funding limited to a one-year study period, we
sought to obtain as many responses as possible, contacting families only
indirectly through homeschool organizations. This is considered a pilot
study for a future national study of homeschool children.
Biological mothers of homeschool children ages 6-12
years were asked to serve as respondents in order to standardize data
collection. They were asked to confirm their consent to participate, to
indicate their home state and zip code of residence, and to confirm that
they had biological children ages 6 to 12. This age-range was selected
because children have completed most of their vaccinations by then, and
would have been diagnosed with the common diseases of childhood if they
were to develop them. The communications company Qualtrics (http://qualtrics.com)
hosted the survey website. Mothers were asked to use their children’s
vaccination records to complete the online survey and to check off items
from a list that pertained to them and their child or children,
including pregnancy-related conditions and medications used, birth
histories (including preterm birth—yes or no), vaccinations,
physician-diagnosed illnesses, medications used by the child, and the
use of health services. Vaccination was defined as receipt of one or
more of the recommended vaccines. NDD, a derived outcome measure, was
defined as a diagnosis of one or more of the following: Autism Spectrum
Disorder (ASD), Attention Deficit Hyperactivity Disorder (ADHD), and a
learning disability. Only closed-ended questions were used. The data
were analyzed using SAS (Version 9.3) to determine the strength of
associations between vaccination and health outcomes in terms of odds
ratios (OR) and 95% Confidence Intervals (CI). Odds ratios describe the
strength of the association between two categorical variables measured
simultaneously and are appropriate measures of that relationship in a
cross-sectional study [49].
Recruitment and informed consent
To increase trust and community engagement,
homeschool organizational leaders were asked to sign Memoranda of
Agreement and to provide the total number of member families. This was
an attempt to interest and recruit as many homeschool families as
possible. Non-responding organizations were sent a second email notice,
but few provided the requested information. Follow-up calls to the
leaders suggested that they had contacted their members about the study.
The online survey remained open for three months in the summer of 2012.
Financial incentives to complete the survey were neither available nor
offered. The questionnaire required only factual, binary responses,
allowing for rapid data entry, with the aim of improving both response
and completion rates. The introductory letter and survey questions were
stated in a neutral way so that, if biases existed, they would be evenly
distributed across comparison groups. Our letter to parents began:
“Dear Parent, This study concerns a major
current health question: namely, whether vaccination is linked in any
way to childrens long-term health. Vaccination is one of the greatest
discoveries in medicine, yet little is known about its long-term impact.
The objective of this study is to evaluate the effects of vaccination
by comparing vaccinated and unvaccinated children in terms of a number
of major health outcomes …”
The survey yielded a sample of 666 children, of
whom 261 (39%) were unvaccinated and 51 (7.7%) were born preterm. Fifty
children (7.5%) had a neurodevelopmental disorder (NDD). The overall
diagnostic category of NDD was created for analytic purposes in view of
the relatively small number of children with the individual diagnoses,
and because the diagnoses of LD, ADHD and ASD are closely related and
overlapping [50]; that is, about 50% of children with ASD meet the
diagnostic criteria for ADHD [51]. In this study the most common
diagnoses were LD only (n = 15), ADHD only (n = 9), and ASD only (n =
9), followed by various combinations of these diagnoses (Figure 1).
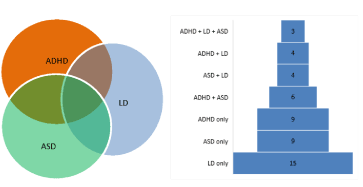
Figure 1. The overlap and distribution of physician-diagnosed neurodevelopmental disorders, based on mothers’ reports.
Table 1 shows the characteristics of the survey
respondents. Mothers averaged about 40 years of age, were typically
white, college graduates, Christian and married, with household incomes
between $50,000 and $100,000. The children as a group were similarly
mostly white (88%), with a slight preponderance of females (52%). With
regard to vaccination status, 261 (39%) were unvaccinated, 208 (31%)
were partially vaccinated, and 197 (30%) had received all of the
recommended vaccinations. All data analyses are based on these numbers.
Table 1. Characteristics of the respondents a
|
|
|
Mean (SD)a |
Age (n=407) |
40.59 (6.7) |
|
Number (%)a |
Race |
|
White |
382 (92.5) |
Non-White |
21 (7.6) |
Total |
413 |
Education |
|
High School Graduate or Less |
35 (8.5) |
Some College |
114 (27.5) |
College Graduate |
187 (45.2) |
Post-Graduates |
78 (18.5) |
Total |
414 |
Total Gross Household Income |
|
< $49,999 |
123 (30.8) |
$50,000-100,000 |
182 (45.5) |
> $100,000 |
95 (23.8) |
Total |
400 |
Religious Affiliation |
|
Christianity |
375 (91.2) |
Non-Christianity |
36 (8.8) |
Total |
411 |
Marital Status |
|
Married |
386 (93.7) |
Not Married |
26 (6.3) |
Total |
412 |
a Missing observations are excluded.
Summary of the initial findings
To summarize the initial results of the study [48],
vaccinated children were significantly less likely than the
unvaccinated to have been diagnosed with chickenpox and pertussis, but
significantly more likely to have been diagnosed with pneumonia, otitis
media, allergies and NDD (that is, ASD, ADHD, and/or a learning
disability). The vaccinated were also more likely to use allergy
medication, to have had myringotomies with tube placement, visited a
doctor for a health problem in the previous year, and been hospitalized
at some time in the past.
The second aim of the study was to determine
whether the association found between vaccination and NDD remained
significant after controlling for other measured factors. The factors
associated with NDD in unadjusted regression analyses were vaccination
(OR 3.7, 95% CI: 1.7, 7.9), male gender (OR 2.1, 95% CI: 1.1, 3.8),
adverse environment (defined as living within 1-2 miles of a furniture
manufacturing factory, lumber factory, waste site or landfill) (OR 2.9,
95% CI: 1.2, 7.4), maternal use of antibiotics in pregnancy (OR 2.3, 95%
CI: 1.1, 4.8), and preterm birth (OR 4.9, 95% CI: 2.4, 10.3). After
adjustment, the factors that remained significantly associated with NDD
were vaccination (OR 3.1, 95% CI: 1.4, 6.8), male gender (OR 2.3, 95%
CI: 1.2, 4.3), and preterm birth (OR 5.0, 95% CI: 2.3, 11.6). However,
in a final adjusted model with interaction, vaccination, but not preterm
birth, remained associated with NDD, while the interaction of preterm
birth and vaccination was associated with a 6.6-fold increased odds of
NDD (95% CI: 2.8, 15.5), suggesting a synergistic effect.
As noted, initial bivariate analyses suggested that
NDD was significantly associated both with preterm birth (OR 4.9, 95%
CI: 2.4, 10.3) and vaccination (OR 3.7, 95% CI: 1.7, 7.9), and more
strongly so with preterm birth than vaccination (see Table 2, below).
Vaccination was also significantly associated with the specific
diagnoses of learning disability (OR 5.2, 95% CI: 1.5, 17.5), ADHD (OR
4.3, 95% CI: 1.2, 14.5), Autism Spectrum Disorder (OR 4.3, 95% CI: 1.2,
14.5) as well as the combined diagnosis of NDD (OR 3.7, 95% CI: 1.7,
7.9) (Table 3, below).
Table 2. Unadjusted associations between preterm birth, vaccination, and neurodevelopmental disorders (NDD)
|
Neurodevelopmental Disorders |
Chi-Square |
OR (95% CI) |
P-value |
Yes n (%)a |
No n (%)b |
Preterm birth |
|
|
|
|
|
Yes |
12 (24.0) |
37 (6.0) |
22.9 |
4.9 (2.4-10.3) |
<0.001 |
No |
38 (76.0) |
578 (93.8) |
|
Vaccination Status |
|
|
|
|
|
Yes |
42 (84.0) |
363 (58.9) |
12.2 |
3.7 (1.7-7.9) |
< 0.001 |
No |
8 (16.0) |
253 (41.1) |
aValues in parentheses indicate % of total (n=50).
bValues in parentheses indicate % of totals for respective factors.
Table 3. Vaccination status and types of NDD
Condition |
Vaccination Status |
n (%) |
OR (95% CI) |
P-value* |
ADHD |
Vaccinated (N=405) |
19 (4.69) |
4.3 (1.3, 14.5) |
0.013 |
|
Unvaccinated (n=261) |
3 (1.15) |
|
|
|
|
|
|
|
ASD |
Vaccinated (N=405) |
19 (4.69) |
4.3 (1.2, 14.5) |
0.013 |
|
Unvaccinated (n=261) |
3 (1.15) |
|
|
|
|
|
|
|
Learning Disability |
Vaccinated (N=405) |
23 (5.68) |
|
|
|
Unvaccinated (n=261) |
3 (1.15) |
5.2 (1.5, 17.5) |
0.003 |
|
|
|
|
|
Any NDD |
Vaccinated (N=405) |
42 (10.37) |
3.7 (1.7, 7.9) |
0.005 |
|
Unvaccinated (n=261) |
- (3.03)
|
|
|
* From Fisher’s exact test.
These findings suggested that preterm birth and
vaccination could be independent risk factors for NDD. However, since
most preterm infants receive the same vaccinations on the same schedule
as those recommended for term infants, interpretation of the findings
remains unclear.
Interactions between preterm birth, vaccination and NDD
Given the apparent synergism in the combination of
vaccination and preterm birth on NDD found in regression analyses [48],
and the relatively small numbers available for analysis, this report
presents additional findings on the association and interaction between
preterm birth (yes, no), vaccination status (yes, no) and NDD (yes, no).
Stratified analyses with Odds Ratios and 95% Confidence Intervals were
used to quantify the strength of the associations. The analytic process
can be envisioned as a 2 X 2 table with the cells in Row 1 labeled A and
B, and those in Row 2 labeled C and D. The odds ratio is calculated by
the formula AD/BC. Here we examine different combinations of preterm
birth and vaccination and their association with NDD. Calculations based
on the data in Table 4 (below) suggest a complex picture of the
association between prematurity, vaccination and NDD.
Table 4. Preterm birth and vaccination status among children with NDD and controls
Neurodevelopmental Disorders |
Yes |
No |
|
Preterm |
Not Preterm |
Preterm |
Not Preterm |
Totals |
Vaccinated |
12 |
30 |
25 |
337 |
404 |
Not vaccinated |
0 |
8 |
12 |
241 |
261 |
Totals |
12 |
38 |
37 |
578 |
665 |
Most children in the sample were vaccinated and not
preterm (n=367; 55%). The second largest group comprised those who were
neither vaccinated nor preterm (n=249; 37%); the third largest
comprised those who were preterm and vaccinated (n=37; 6%), and the
smallest group those who were preterm and unvaccinated (n=12; 2%).
While acknowledging that our study group is
relatively small and not a representative sample of U.S. children, the
following observations are noted. First, of the 37 children who were
both preterm and vaccinated (P/V), 12 (32%) had an NDD, consistent with
studies suggesting that a high proportion of preterm infants are later
diagnosed with ASD [18-20]. Second, of the 12 children who were preterm
but unvaccinated (P/V-), none had an NDD. Third, among the 367 children
in the sample who were not preterm but vaccinated (P-/V), 30 (8%) had an
NDD. Fourth, of the 249 children who were neither preterm nor
vaccinated (P-/V-), only 8 (3%) had an NDD. These observations suggest
that birth history strongly affects the likelihood of NDD in vaccinated
children, given that the combination of preterm birth and vaccination
accounts for a substantial proportion of NDD diagnoses in the overall
sample. In contrast, cases of NDD are under-represented in preterm but
unvaccinated children. These suggestions are further supported and
amplified by analyses of the odds of NDD given various combinations of
preterm birth and vaccination (see Table 5).
Table 5. Association between combinations of preterm birth and vaccination status, and neurodevelopmental disorders (NDD)
Combinations of Exposures |
NDD |
OR (95% CI) |
P-value* |
|
Yes |
No |
|
|
1. Preterm and Unvaccinated (P/V-) |
0 |
12 |
1.14 (0.1, 20.8)** |
1 |
Not Preterm and Unvaccinated (P-/V-) |
8 |
241 |
|
|
|
|
|
|
|
2. Not Preterm and Vaccinated (P-/V) |
30 |
337 |
2.7 (1.2, 6.0) |
0.012 |
Not Preterm and Unvaccinated (P-/V-) |
8 |
241 |
|
|
|
|
|
|
|
3. Preterm and Vaccinated (P/V) |
12 |
25 |
5.4 (2.5, 11.9) |
< 0.001 |
Not Preterm and Vaccinated (P-/V) |
30 |
337 |
|
|
|
|
|
|
|
4. Preterm and Vaccinated (P/V) |
12 |
25 |
12.3 (0.67, 224.2)** |
0.024 |
Preterm and Unvaccinated (P/V-) |
0 |
12 |
|
|
|
|
|
|
|
5. Preterm and Vaccinated (P/V) |
12 |
25 |
14.5 (5.4, 38.7) |
< 0.001 |
Not Preterm and Unvaccinated (P-/V-) |
8 |
241 |
|
|
* From Fisher’s exact test.
** Calculated by adding 0.5 to each cell because of zero count.
Table 5 shows the following:
1) Preterm birth without vaccination (P/V-) was not associated with NDD.
2) Term birth with vaccination (P-/V) was associated with a significant 2.7-fold increase in the odds of NDD.
3) Preterm birth with vaccination (P/V) was
associated with a significant 5.4-fold increase in the odds of NDD
compared to the odds of NDD given term birth and vaccination (P-/V).
4) Preterm birth with vaccination (P/V) was
associated with a nonsignificant 12.3-fold increased odds of NDD
compared to preterm birth without vaccination (P/V-) (not technically
significant because no child in the sample with an NDD was both preterm
and unvaccinated).
5) Preterm birth with vaccination (P/V) was
associated with a significant 14.5-fold increased odds of NDD compared
to being neither preterm nor vaccinated (P-/V-).
Figure 2 depicts the findings reported in Table 5.
In summary, the results suggest that: preterm birth without vaccination
is not associated with NDD; vaccination (in a term infant) is associated
with a 2.7-fold increased odds of NDD, compared to an unvaccinated
child born at term (P-/V-); and the combination of preterm birth and
vaccination (P/V) is associated with progressively increased odds of NDD
(depending on birth history and vaccination status), with a 5.4-fold
increase compared to vaccination alone, a 12.3-fold (nonsignificant)
increase compared to preterm birth alone (i.e., unvaccinated),
and a 14.5-fold increase compared to term birth without vaccination.
These results (depicted in Figure 2, below) suggest that preterm birth
without vaccination is not associated with NDD whereas vaccination is
(regardless of birth history), and that vaccination coupled with preterm
birth greatly increases the odds of NDD compared to vaccination alone.
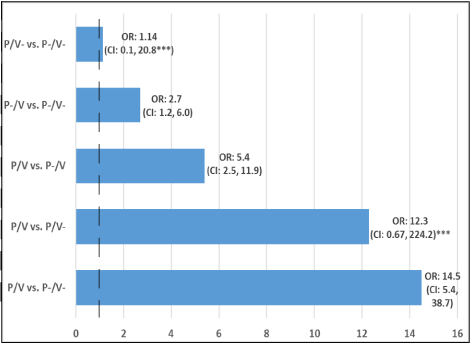
Figure 2. Combinations of Preterm birth and Vaccination Status* and the Odds Ratio of Neurodevelopmental Disorders with 95% CI**
Prematurity is a known risk factor for
neurodevelopmental disorders, with 8% to 27% of extremely preterm
infants showing symptoms of autism at 6 years of age [20]. Late preterm
infants are also reportedly more prone to long-term neurologic sequelae
than previously recognized [16,17]. Premature infants typically receive
the same doses of recommended vaccines and on the same schedule as term
infants, yet the possible role of vaccination in preterm-associated NDD
has not been investigated. A unique feature of this study is that it
included birth history and pregnancy experiences, based on mothers’
reports. The present analysis focused on the association and possible
interaction of preterm birth (yes, no) and vaccination (yes, no) in
relation to NDD (yes, no).
In our initial report [48], logistic regression
analyses revealed that both preterm birth and vaccination (receipt of
one of more of the recommended vaccines) were significantly associated
with NDD after controlling for other factors, suggesting independent
effects. However, in a final regression model with interaction, preterm
birth combined with vaccination was associated with a 6.6-fold increased
odds of NDD, suggesting a synergistic effect.
This second report focused on the association
between preterm birth, vaccination and NDD. Because of the relatively
small numbers, stratified analyses with Odds Ratios and 95% Confidence
Intervals were used to examine and quantify different combinations of
preterm birth and vaccination in relation to NDD. Vaccination was found
to be significantly and independently associated with NDD, whereas
preterm birth without vaccination was not. However, vaccination coupled
with preterm birth greatly increased the odds of NDD over that of
vaccination alone, especially compared to being born at term and
unvaccinated, suggesting that vaccination may adversely affect
neurodevelopmental outcomes in preterm infants. Indeed, the apparent
synergism between preterm birth and vaccination in regard to NDD
suggests the possibility that rising rates of NDD could be driven in
part by the vaccination of growing numbers of late preterm newborns, the
latter of which account for 74% of all preterm birth and about 8% of
total births [53].
While additional studies are needed to verify and
explain the present findings, a tentative hypothesis of the mechanisms
linking preterm birth and vaccination with NDD is outlined as follows.
Receipt of one or more vaccines could precipitate NDD in some preterm
infants by exacerbating a preexisting inflammatory state associated with
prematurity, leading to hepatic encephalopathy and hypoxic-ischemic
brain damage. Impaired liver function is a predisposing factor for
preterm birth [54,55] and the latter is associated with increased risks
of hypoxic-ischemic brain injury [56]. A possible biochemical basis for
vaccination-associated NDD in preterm infants could involve the spillage
of a membranolytic biliary metabolite from the maternal liver into the
circulation and its transfer to the fetus, contributing thereby to the
pathogenesis of preterm birth itself [55] and possibly being further
increased to neurotoxic concentrations by the impact of vaccination on
the infant’s liver. Consistent with this hypothesis, liver dysfunction
is reported as an adverse effect of vaccination [57] and as a feature of
children with autism [58,59]. Furthermore, hyperbilirubinemia is
associated with hypoxic-ischemic brain damage [60] and is a feature of
the preterm infant as well as children with later-onset cognitive
disorders and ASD [61,62].
Strengths of the study include: the relatively
large sample of unvaccinated children (N=261); the demographically
homogeneous sample of mainly white, higher-income and college-educated
homeschooling families, in which the children studied were 6 to 12 years
of age; and the recruitment of biological mothers as respondents, which
made it possible to test hypotheses about the role of pregnancy-
related factors, birth history and vaccination in specific conditions.
Contact information on the families and the membership of homeschool
organizations was unavailable, which meant that neither the number of
homeschool families contacted nor the survey response rate could be
determined. However, the study was not intended to be a representative
survey of homeschool children but to achieve a sample of sufficient size
to test for significant differences in outcomes. Homeschoolers were
targeted for the study because their vaccination completion rates are
lower than those of children in general. Although respondents were
self-selected, efforts were made to reduce or eliminate biases of
several kinds. To minimize recall bias, respondents were asked to use
their child’s vaccination records; to enhance reliability, closed-ended
questions were used; to enhance validity, parents were asked to report
only physician-diagnosed illnesses.
Study limitations include the relatively small
number of preterm children and children with NDD. To preserve anonymity,
the reported health outcomes could not be validated by clinical
records. However, self-reports are accepted as a valid proxy for
official records when the latter are unavailable [63]. A further
potential limitation is that morbidity may have been under-estimated in
unvaccinated children, as they were less likely than the vaccinated to
see a physician for a routine checkup in the past year (57.6% vs. 37.2%,
p <0.001; OR 2.3, 95% CI: 1.7, 3.2). This could be due to the fact
that such visits usually involve vaccinations, which non-vaccinating
families would be expected to refuse. However, unvaccinated children
were more likely than the vaccinated to be diagnosed with chickenpox and
pertussis, which would have involved one or more visits to the
pediatrician. This suggests that observed differences in health outcomes
were not due to under-ascertainment of disease.
This study compared the birth histories and health
outcomes of vaccinated and unvaccinated children and sought to determine
the association, if any, between vaccination, preterm birth and
neurodevelopmental disorders (NDD). Vaccination (i.e., receipt
of one of more of the recommended vaccines) was significantly associated
with NDD, while preterm birth without vaccination was not. Preterm
birth coupled with vaccination, however, was associated with a
synergistic increase in the odds of NDD, suggesting the possibility that
vaccination could precipitate adverse neurodevelopmental outcomes in
preterm infants. These results provide clues to the epidemiology and
causation of NDD but question the safety of current vaccination programs
for preterm infants. Further research is needed to validate and
investigate these findings in order to optimize the impact of vaccines
on children’s health.
We thank all those who helped fund the study,
provided insights and reviews of earlier drafts and offered helpful
suggestions and support throughout the research project. We also thank
the homeschool organizations and the mothers who participated in the
survey.
Conflict of interest
The first author has advocated for further research
on the health outcomes of routine vaccination. None of the authors has a
financial conflict of interest to declare.
Author contributions
ARM designed the study, contributed to data
analysis and interpretation, and wrote successive drafts of the paper.
AB contributed to data analyses and edited the paper. BJ contributed to
data analyses and editing. BR designed the study, contributed to data
collection, and edited the paper. All authors read and approved the
final version of the paper.
Funding sources
This study was supported by grants from Generation
Rescue, Inc., and the Children’s Medical Safety Research Institute. Both
are charitable organizations that support research on children’s health
and safety. The funders had no role or influence on the design and
conduct of the research or the preparation of reports.
Disclaimer
This study, approved by the Institutional Review
Board of Jackson State University, was completed prior to Dr. Mawson’s
tenure-track appointment at Jackson State University.
- Meldrum SJ, Strunk T, Currie A, Prescott SL,
Simmer K, et al. (2013) Autism spectrum disorder in children born
preterm-role of exposure to perinatal inflammation. Front Neurosci 7: 123. [Crossref]
- Pyhälä R, Hovi P, Lahti M, Sammallahti S, Lahti
J, et al. (2014) Very low birth weight, infant growth, and
autism-spectrum traits in adulthood. Pediatrics 134: 1075-1083. [Crossref]
- Dudova I, Kasparova M, Markova D, Zemankova J,
Beranova S, et al. (2014) Screening for autism in preterm children with
extremely low and very low birth weight. Neuropsychiatr Dis Treat 10: 277-282. [Crossref]
- Atkinson WL, Pickering LK, Schwartz B, Weniger
BG, Iskander JK, et al. (2002) Centers for Disease Control and
Prevention. General recommendations on immunization. Recommendations of
the Advisory Committee on Immunization Practices (ACIP) and the American
Academy of Family Physicians (AAFP). MMWR Recomm Rep 51: 1-35. [Crossref]
- Esposito S, Serra D, Gualtieri L, Cesati L, Principi N (2009) Vaccines and preterm neonates: why, when, and with what. Early Hum Dev 85: S43-45. [Crossref]
- Omeñaca F, Merino JM, Tejedor JC,
Constantopoulos A, Papaevangelou V, et al. (2011) Immunization of
preterm infants with 10-valent pneumococcal conjugate vaccine. Pediatrics 128: e290-298. [Crossref]
- Blencowe H, Lee AC, Cousens S, Bahalim A, Narwal
R, et al. (2013) Preterm birth-associated neurodevelopmental
impairment estimates at regional and global levels for 2010. Pediatr Res 74 Suppl 1: 17-34. [Crossref]
- http://www.cdc.gov/vaccinesafety/concerns/autism/ (Accessed July 19, 2016).
- DeStefano F, Price CS, Weintraub ES (2013)
Increasing exposure to antibody-stimulating proteins and polysaccharides
in vaccines is not associated with risk of autism. J Pediatr 163: 561-567. [Crossref]
- http://www.cdc.gov/vaccinesafety/pdf/iso-final-scientific_agenda-nov-10.pdf (Accessed July 19, 2016).
- Institute of Medicine (2012) Adverse Effects of Vaccines: Evidence and Causality. The National Academies Press, Washington, DC.
- Institute of Medicine (2013) The childhood
immunization schedule and safety: Stakeholder concerns, scientific
evidence, and future studies: National Academies Press, Washington, DC.
- Maglione MA, Das L, Raaen L, Smith A, Chari R,
et al. (2014) Safety of vaccines used for routine immunization of U.S.
children: a systematic review. Pediatrics 134: 325-337. [Crossref]
- Taylor LE, Swerdfeger AL, Eslick GD (2014)
Vaccines are not associated with autism: an evidence-based meta-analysis
of case-control and cohort studies. Vaccine 32: 3623-3629. [Crossref]
- Jain A, Marshall J, Buikema A, Bancroft T, Kelly
JP, et al. (2015) Autism occurrence by MMR vaccine status among US
children with older siblings with and without autism. JAMA 313: 1534-1540. [Crossref]
- Jarjour IT (2015) Neurodevelopmental outcome after extreme prematurity: a review of the literature. Pediatr Neurol 52: 143-152. [Crossref]
- Loftin RW, Habli M, Snyder CC, Cormier CM, Lewis DF, et al. (2010) Late preterm birth. Rev Obstet Gynecol 3: 10-19. [Crossref]
- Johnson S, Hollis C, Kochhar P, Hennessy E, Wolke D, et al. (2010) Autism spectrum disorders in extremely preterm children. J Pediatr 156: 525-531. [Crossref]
- Developmental Disabilities Monitoring Network
Surveillance Year 2010 Principal Investigators; Centers for Disease
Control and Prevention (CDC) (2014) Prevalence of autism spectrum
disorder among children aged 8 years - autism and developmental
disabilities monitoring network, 11 sites, United States, 2010. MMWR Surveill Summ 63: 1-21.
- Padilla N, Eklöf E, Mårtensson GE, Bölte S,
Lagercrantz H, et al. (2015) Poor brain growth in extremely preterm
neonates long before the onset of autism spectrum disorder symptoms. Cereb Cortex 27: 1245-1252. [Crossref]
- Bonhoeffer J, Siegrist CA, Heath PT (2006) Immunisation of premature infants. Arch Dis Child 91: 929-935. [Crossref]
- Schulzke S, Heininger U, Lücking-Famira M,
Fahnenstich H (2005) Apnoea and bradycardia in preterm infants following
immunisation with pentavalent or hexavalent vaccines. Eur J Pediatr 164: 432-435. [Crossref]
- Lee J, Robinson JL, Spady DW (2006) Frequency of
apnea, bradycardia, and desaturations following first
diphtheria-tetanus-pertussis-inactivated polio-Haemophilus influenza
type B immunization in hospitalized preterm infants. BMC Pediatr 6: 20. [Crossref]
- Pfister RE, Aeschbach V, Niksic-Stuber V, Martin
BC, Siegrist CA (2004) Safety of DTaP-based combined immunization in
very-low-birth-weight premature infants: frequent but mostly benign
cardiorespiratory events. J Pediatr 145: 58-66. [Crossref]
- Sen S, Cloete Y, Hassan K, Buss P (2001) Adverse events following vaccination in premature infants. Acta Paediatr 90: 916-920. [Crossref]
- DeMeo SD, Raman SR, Hornik CP, Wilson CC, Clark
R, et al. (2015) Adverse events after routine immunization of extremely
low-birth-weight infants. JAMA Pediatr 169: 740-745. [Crossref]
- Halperin SA1, Tapiéro B, Dionne M, Meekison W,
Diaz-Mitoma F, et al. (2014) Safety and immunogenicity of a toddler dose
following an infant series of a hexavalent diphtheria, tetanus,
acellular pertussis, inactivated poliovirus, Haemophilus influenzae type
b, hepatitis B vaccine administered concurrently or at separate visits
with a heptavalent pneumococcal conjugate vaccine. Pediatr Infect Dis J 33: 73-80. [Crossref]
- Centers for Disease Control and Prevention (CDC)
(2007) Vaccination coverage among children in kindergarten--United
States, 2006-07 school year. MMWR Morb Mortal Wkly Rep 56: 819-821. [Crossref]
- Centers for Disease Control and Prevention (CDC)
(2013) Vaccination coverage among children in kindergarten - United
States, 2012-13 school year. MMWR Morb Mortal Wkly Rep 62: 607-612. [Crossref]
- http://www.cdc.gov/vaccines/vac-gen/whatifstop.htm (Accessed July 19, 2016).
- Whitney CG, Zhou F, Singleton J, Schuchat A;
Centers for Disease Control and Prevention (CDC) (2014) Benefits from
immunization during the vaccines for children program era - United
States, 1994-2013. MMWR Morb Mortal Wkly Rep 63: 352-355. [Crossref]
- Sienkiewicz D, Kulak W, Okurowska-Zawada B, Paszko-Patej G (2012) Neurologic adverse events following vaccination. Prog Health Sci 2: 129-141.
- http://www.hrsa.gov/vaccinecompensation/data.html (Accessed July 19, 2016).
- Kessler DA (1993) Introducing MEDWatch. A new approach to reporting medication and device adverse effects and product problems. JAMA 269: 2765-2768. [Crossref]
- Aaby P, Whittle H, Benn CS (2012) Vaccine programmes must consider their effect on general resistance. BMJ 344: e3769. [Crossref]
- http://www.hhs.gov/sites/default/files/nvpo/vacc_plan/2010-Plan/nationalvaccineplan.pdf (Accessed July 19, 2016).
- Aaby P, Benn C, Nielsen J, Lisse IM, Rodrigues
A, et al. (2012) Testing the hypothesis that
diphtheria-tetanus-pertussis vaccine has negative non-specific and
sex-differential effects on child survival in high-mortality countries. BMJ Open 2: e000707. [Crossref]
- Garly ML, Jensen H, Martins CL, Balé C, Baldé
MA, et al. (2004) Hepatitis B vaccination associated with higher female
than male mortality in Guinea-Bissau: an observational study. Pediatr Infect Dis J 23: 1086-1092. [Crossref]
- Benn CS, Netea MG, Selin LK, Aaby P (2013) A small jab - a big effect: nonspecific immunomodulation by vaccines. Trends Immunol 34: 431-439. [Crossref]
- Sørup S, Benn CS, Poulsen A, Krause TG, Aaby P,
et al. (2014) Live vaccine against measles, mumps, and rubella and the
risk of hospital admissions for nontargeted infections. JAMA 311: 826-835. [Crossref]
- http://www.cdc.gov/vaccines/schedules/easy-to-read/index.html (Accessed July 19, 2016).
- Choi BK, Manning ML (2010) The immunization status of home-schooled children in America. J Pediatr Health Care 24: 42-47. [Crossref]
- Ray BD (2010) Academic achievement and demographic traits of homeschool students: a nationwide study. J Acad Leadership 8: 1.
- http://www.census.gov/library/publications/2011/compendia/statab/131ed.html(Accessed July 19, 2016).
- https://nces.ed.gov/fastfacts/display.asp?id=91 (Accessed July 19, 2016).
- http://nces.ed.gov/programs/digest/d13/tables/dt13_206.10.asp(Accessed July 19, 2016)
- http://nces.ed.gov/pubsearch (Accessed July 19, 2016).
- Mawson AR, Ray BD, Bhuiyan AR, Jacob B (2017)
Pilot comparative study on the health of vaccinated and unvaccinated
U.S. children. J Transl Sci 3: 1-12.
- Zocchetti C, Consonni D, Bertazzi PA (1997)
Relationship between prevalence rate ratios and odds ratios in
cross-sectional studies. Int J Epidemiol 26: 220-223. [Crossref]
- Surén P, Bakken IJ, Aase H, Chin R, Gunnes N, et
al. (2012) Autism spectrum disorder, ADHD, epilepsy, and cerebral palsy
in Norwegian children. Pediatrics 130: e152-158. [Crossref]
- Nelson CA (2015) Commentary: Developmental origins of autism and ADHD--a commentary on Johnson et al. (2015). J Child Psychol Psychiatry 56: 248-250. [Crossref]
- Kurosky SK, Davis KL, Krishnarajah G (2016) Completion and compliance of childhood vaccinations in the United States. Vaccine 34: 387-394. [Crossref]
- Loftin RW, Habli M, Snyder CC, Cormier CM, Lewis DF, et al. (2010) Late preterm birth. Rev Obstet Gynecol 3: 10-19. [Crossref]
- Hagström H, Höijer J, Ludvigsson JF, Bottai M,
et al. (2016) Adverse outcomes of pregnancy in women with non-alcoholic
fatty liver disease. Liver Int 36: 268-274. [Crossref]
- Mawson AR (2016) A Role for the Liver in Parturition and Preterm Birth. J Transl Sci 2: 154-159. [Crossref]
- Gopagondanahalli KR, Li J, Fahey MC, Hunt RW, Jenkin G, et al. (2016) Preterm Hypoxic-Ischemic Encephalopathy. Front Pediatr 4: 114. [Crossref]
- Pellegrino P, Perrotta C, Clementi E, Radice S
(2015) Vaccine-Drug Interactions: Cytokines, Cytochromes, and Molecular
Mechanisms. Drug Saf 38: 781-787. [Crossref]
- Guevara-Campos J, González-Guevara L,
Puig-Alcaraz C, et al. (2013) Autism spectrum disorders associated to a
deficiency of the enzymes of the mitochondrial respiratory chain. Metab Brain Dis 28: 605-612. [Crossref]
- Weissman JR, Kelley RI, Bauman ML, Cohen BH,
Murray KF, et al. (2008) Mitochondrial disease in autism spectrum
disorder patients: a cohort analysis. PLoS One 3: e3815. [Crossref]
- Wusthoff CJ, Loe IM (2015) Impact of bilirubin-induced neurologic dysfunction on neurodevelopmental outcomes. Semin Fetal Neonatal Med 20: 52-57. [Crossref]
- Maimburg RD, Bech BH, Vaeth M, Møller-Madsen B,
Olsen J (2010) Neonatal jaundice, autism, and other disorders of
psychological development. Pediatrics 126: 872-878.
- Watchko JF, Tiribelli C (2013) Bilirubin-induced neurologic damage--mechanisms and management approaches. N Engl J Med 369: 2021-2030. [Crossref]
- Short ME, Goetzel RZ, Pei X, Tabrizi MJ,
Ozminkowski RJ, et al. (2009) How accurate are self-reports? Analysis of
self-reported health care utilization and absence when compared with
administrative data. J Occup Environ Med 51: 786-796. [Crossref]

